Remarkable Hypokalemia among Sudanese
Patients with Jaundice
Abdel-Moniem
MS. Arjabey, Bashir A. Bashir
Introduction
Potassium is one of the most noteworthy
body particles. About 98% of the body's potassium is intracellular [1]. The
proportion of intracellular to extracellular potassium is major in marking the
cellular membrane [2]. The kidney controls the potassium homeostasis, and an
abundance of potassium is discharged in the urine. A diminished level of
potassium less than 3.5 mEq/l is called hypokalemia.
Hypokalemia may have come about because of numerous conditions, such as renal
impairment, gastrointestinal losses, inadequate diet, medications and
transcellular move [3]. The judgment of the etiology of hypokalemia is
mandatory prior initiating specific therapy [4]. Firstly, we should ensure that
this hypokalemia is not spurious. This will assist to avert the inappropriate
management that can conduce to adverse outcomes. Spurious hypokalemia refers to
an artifactual decrease in serum potassium levels that do not superpose to
their actual systemic values [5]. On the other hand, jaundice is a yellow stain
that takes office when the bilirubin concentration in the blood rises more than
(3 mg/dl) and the bilirubin is precipitated in the skin and sclera of the
optics. Whereas Icterus describes the plasma and tissue. Jaundice can be
assorted into pre-hepatic (hemolytic), hepatic, and post-hepatic (obstructive)
jaundice. Patients with jaundice particularly the obstructive type are at high
risk for developing renal impairment which may be a life-threatening
complication. A former study has been described that the severe jaundice was
related to hypokalemia in a proportion of 63% and hyponatremia 56% [6]. This
work has been held away to evaluate the potassium levels in patients with
jaundice.
Materials and Methods
A cross-sectional study included 90
patients with jaundice divided as follows; 30 patients with pre-hepatic
jaundice, 30 patients with hepatic jaundice, 30 patients with post-hepatic
(obstructive) jaundice admitted to a laboratory unit of Port Sudan teaching
hospital during the period from the 14th July 2008 to the 5th April 2009. The
cases were picked up among the admitted patients who had indications suggestive
of jaundice with serum bilirubin levels more than 2 mg/dl and they looked for
medicinal exhortation as long as 3 weeks of disease.
Clinically, a general survey and scrutiny of the abdomen, respiratory system,
nervous system, and cardiovascular system were taken. Serum potassium and
bilirubin concentration levels were assessed.
Inclusion and exclusion criteria
Patients with jaundice documented
by laboratory findings, ultrasonography, and magnetic resonance imaging (MRI)
were enrolled. Patients with pre-existing renal pathology or other causes of
hypokalemia were excluded from the study.
Study sample
Blood samples were withdrawn from
each member of the study. 3 ml (non-hemolyzed) venous blood specimens were
collected in plain containers (without aggregator). The specimens were
forwarded to obtain serum using centrifugation under standard temperature. The
laboratory investigations were performed by a fully automated chemistry
analyzer (Selectra pro S, Switzerland).
Data analysis
The gauging of laboratory chemistry
tests of patients with jaundice was statistically tested by a one-way ANOVA and
Chi-square test whichever was relevant. Linear regression was used to adjust
confounding variable between potassium levels and bilirubin concentration.
Significance value P < 0.05 were considered statistically significant. Data
were analyzed using statistical package for social science (SPSS 24.0 version,
IBN, Chicago, USA).
Ethical Clearance
This study was endorsed by the
regional ethical review committee. Informed consent was taken from every
participant of the study.
Results
This prospective study was carried
out during the 8-month period from 2008 to 2009. 90 patients with jaundice and
along with 30 controls were enrolled. 55 (61.1%) were males and 35 (38.9%) were
females among the Icterus patients, with the mean age being 39.6 +/- 17.1
years. While 21 (70%) were males and 9 (30%) were females among the control,
with the mean age being 34.6 +/- 13.9 years. The main findings for all members,
encompassing the Icterus profiles and potassium levels are presented in (Table
1). The mean of Icterus profiles was significantly higher in patients than the
control (P < 0.000). While the mean potassium levels were significantly
lower in patients compared to the control (P < 0.000).
Peak conjugated bilirubin
concentration was observed in all hepatic and obstructive jaundice. Whereas the
unconjugated bilirubin concentration was also peaked in all hemolytic and
hepatic jaundice. Normal unconjugated bilirubin concentration was only detected
in 20 (22.2%) in obstructive jaundice, unlike the conjugated bilirubin
concentration which was noted only in hemolytic jaundice. Potassium levels were
normal in 45(50%) of the Icterus patients, meanwhile 45 (50%) were had
hypokalemia in Icterus patients. No hyperkalemia has been associated with
Icterus patients (Table 2).
Patients with hepatic and
obstructive jaundice had a significantly higher severity of illness as
highlighted by the reduced potassium levels (hypokalemia) (P < 0.000). On
the contrary, patients with hemolytic jaundice had significant slight severity
of sickness owing only to 2 (2.2%) Icterus patients had hypokalemia.
Furthermore, jaundice was significantly associated with hypokalemia, this
association was expressed statistically by regression analysis (Figures 1, 2)
which revealed diminished potassium levels with respect to the onset of
jaundice. Hypokalemia was strongly positively correlated with conjugated
bilirubin concentration (P < 0.000, r; - 0.736) and at one time negatively
correlated with unconjugated bilirubin concentration (P < 0.078/r, - 0.187).
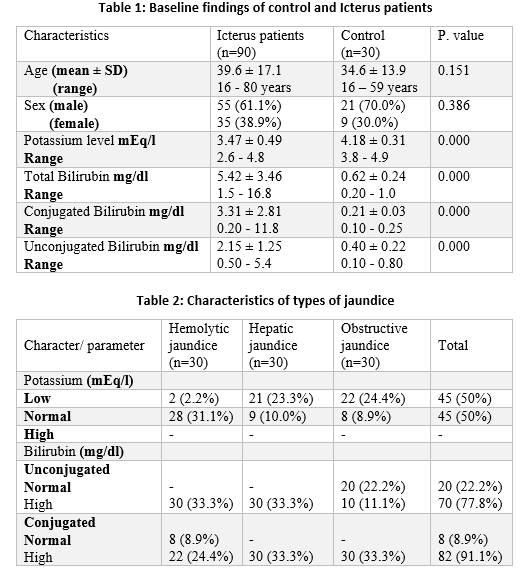
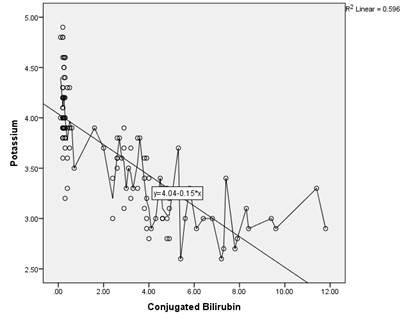
Figure 1: The relationship between potassium level and conjugated
bilirubin concentration
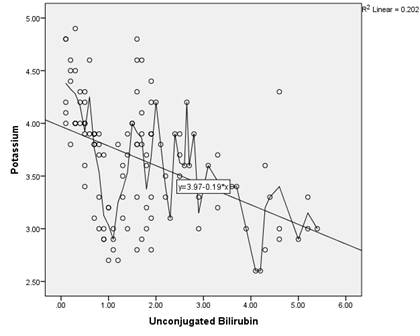
Figure 2: The
relationship between potassium level and unconjugated bilirubin concentration
Discussion
True, in that regard is a paucity
of data in our general vicinity respected to hypokalemia with jaundice.
Consequently, our work revealed that the patients with hepatic and obstructive
jaundice had the peak serum concentration, although there was a slight
presentation of hemolytic jaundice. In the current study, hypokalemia was
significantly observed with intrahepatic and extrahepatic jaundice. These findings
were strongly consistent with Ahmed et al and Souheil
Abu-Assi et al [7, 8].
Hypokalemia is a gravest
complication when associated with jaundice. As mention globally, 50 - 80% of
Icterus patients develop hypokalemia. Moreover, hypokalemia was detected in 45
(50%) of Icterus patients that are relatively concordance with the
international statement [9]. Hypokalemia yields due to locomotion of potassium
from intracellular to extracellular stores. The hydrogen atom outside the cell
moves into the cell to conserve the electroneutrality, consequently, ammonia
outputting increase due to intracellular acidosis in renal tubular cells. The
switched of ammonium is furthered by accompanied contribution of metabolic
alkalosis. Ammonium is a chipped element that cannot pass the blood-brain
septum, whereas ammonia can engage the brain [10].
Gaduputi V in their study
investigates the prognostic findings of hypokalemia in patients with jaundice.
These potential prognostic outcomes such as the blood PH, ammonia level, and stay
duration in the hospital [11]. Nonetheless, hospital accommodations were
significantly longer among Icterus patients with hypokalemia. This finding was
considerably similar to our patients. Furthermore,
they had established an association of hypokalemia with different types of
jaundice. Ahmed et al and Mehboob observed hypokalemia in 34% subjects with
jaundice and intestinal bleeding [7, 12]. Other assorted variety studies
performed in different places showed hypokalemia in cirrhotic patients (33% to
68%) and other liver diseases (6.4%) [7, 12, 13 - 15]. Referred to literature,
numerous different explores completed worldwide have been exhibited variable
level of hypokalemia in patients with chronic liver anomalies [7, 16]. The
organization of diuretics additionally have been created hypokalemia in
patients with liver impairment and ascites [17]. To our knowledge, no study at
the country regarding hypokalemia status among the Icterus patients has been
performed. Due to short of facilities the other compartments of liver function
as well as sodium level and chloride level were not performed in this work. On
the other hand, this study neglected the causes of jaundice, which is a strong
limitation of this inquiry. Nevertheless, wide studies with relative or other
sophisticated method should be viewed in the hereafter.
Conclusion
In light of the aftereffects
of this study, the prevalence of hypokalemia among Icterus patients was high.
Investigations of electrolytes, especially potassium level ought to be requested
for all patients with jaundice to prohibit hypokalemia. Early recognition and
critical remedy of hypokalemia diminish the morbidity and the expenses of the
drugs.
References
[1] Lin SH, Huang CL. Mechanism of thyrotoxic periodic paralysis. J Am Soc Nephrol 2012;23(6):985-988. Available from: http://www.jasn.org/lookup/doi/10.1681/ASN.2012010046 doi: 10.1681/ASN.2012010046. [Google Scholar]
[2] Zacchia M, Abategiovanni ML, Stratigis S, Capasso G. Potassium: From Physiology to clinical Implications. Kidney Dis (Basel 2016;2(2):72-79. Available from: https://www.karger.com/Article/FullText/446268 doi: 10.1159/000446268. [Google Scholar]
[3] Wu KL, Cheng CJ, Sung CC, Tseng MH, Hsu YJ, Yang SS, et al. identification of the causes for Chronic Hypokalemia: importance of Urinary Sodium and Chloride Excretion. Am J Med 2017;130(7):846-855. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0002934317301304 doi: 10.1016/j.amjmed.2017.01.023. [Google Scholar]
[4] Ciulla AP, Lehman DC. . Success! in clinical laboratory science: complete review. 4th ed. Pearson Education; 2010. [Google Scholar]
[5] Liamis G, Liberopoulos E, Barkas F, Elisaf M. Spurious electrolyte disorders: A diagnostic Challenge for Clinicians. Am J Nephrol 2013;38(1):50-57. Available from: https://www.karger.com/Article/FullText/351804 doi: 10.1159/000351804. [Google Scholar]
[6] Wang L, Yu WF. Obstructive jaundice and Perioperation management. Acta Anesthesiologic Taiwanica 2014;52(1):22-29. Available from: https://linkinghub.elsevier.com/retrieve/pii/S1875459714000265 doi: 10.1016/j.aat.2014.03.002. [Google Scholar]
[7] Ahmed I, Amin ZA, Ashraf HM. Determination of factors precipitating encephalopathy in patients with liver cirrhosis. Pak Armed Forces Med J Sep 2006;56(3):284-288. [Google Scholar]
[8] Abu-Assi S, Vlaeevie ZR. Hepatic encephalo-pathy: metabolic consequences of the cirrhois are often reversible. Post graduate Med 2001;109:80. [Google Scholar]
[9] Starr SP, Raines, D "Cirrhosis, , diagnosis, management, and prevention" . . 2011;84(12):1353. [Google Scholar]
[10] Jamali AA, Jamali GM, Jamali AA, Chandio MH, Tanwani BM. Hypokalemia in cirrhotic patients. Indo American Journal of Pharmaceutical Sciences 2018;5(3):1831. [Google Scholar]
[11] Gaduputi V, Chandrala C, Abbas N, Tariq H, Chilimuri S, Balar B. Prognostic significance of hypokalemia in hepatic encephalopathy. Hepatogastroenterology 2014;61(133):1170. [Google Scholar]
[12] Mehboob F. Frequency of risk factors for hepatic encephalopathy in patients of chronic liver disease. Ann King Edward Med Coll 2003;9:29-30. [Google Scholar]
[13] Devrajani BR, Shah SZ, Devrajani T, Kumar D. Precipitating factors of hepatic encephalopathy at a tertiary care hospital Jamshoro, Hyderabad. J Pak Med Assoc 2009;59(10):683-686. [Google Scholar]
[14] Masood N, Rahopoto Q, Gouri A, Munir A. Precipitating factors of hepatic encephalopathy in patients with cirrhosis of liver. Med channel 2010;16(3):376-379. [Google Scholar]
[15] Mumtaz K, Ahmed US, Abid S, Baig N, Hamid S, Jafri W. Precipitating factors and the outcome of hepatic encephalopathy in liver cirrhosis. J Coll Physicians Surg Pak 2010;20(8):514-518. [Google Scholar]
[16] Alam I, Razaullah, Haider I, Humayun M, Taqweem MA, Nisar M . Spectrum of precipitating factors of hepatic encephalopathy in liver cirrhosis. Pakistan J Med Res 2005;44(2):96-100. [Google Scholar]
[17] Sundaram V, Shaikh OS. Hepatic encephalopathy: pathophysiology and emerging therapies. Med. Clin. North Am 2009;93(4):819. [Google Scholar]